COVID-19 And Malaria: Progress at risk
Over the past few months, the COVID-19 pandemic has tested the resilience of health systems across the globe, with devastating impacts on communities everywhere, including here in Britain.
COVID-19 poses an enormous immediate threat to life, and as health services struggle under the extra burden, countries are also being confronted with devastating secondary consequences. For countries with weak health systems, who are already battling deadly diseases such as malaria, the impacts of the pandemic are likely to be even more severe.
Current investments in tackling malaria prevent almost 100 million cases of malaria a year and save close to 600,000 lives. But If we do not sustain efforts to prevent, detect and treat malaria during this time of crisis posed by the COVID-19 pandemic, we risk reversing the hard-won gains that have been made over many years, compromising the health and well-being of millions of people, particularly those most vulnerable to the disease: pregnant women and children. But more than that – we continue to leave countries vulnerable to new pandemics in the future.
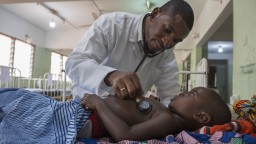
Experience from previous disease outbreaks has shown their hugely disruptive effect on health service delivery and the consequences for diseases such as malaria. When Ebola hit in 2014-2016 in Guinea, Liberia and Sierra Leone, malaria control efforts were severely undermined and led to a massive resurgence in malaria-related illness and death in the three countries.
Recent modelling reports from Imperial College London and WHO suggest the impacts of Covid-19 on malaria deaths could be even more catastrophic. According to these two reports, severe disruption to insecticide-treated net campaigns and other core malaria prevention and treatment activities due to COVID-19 could lead to a doubling in the number of malaria deaths in sub-Saharan Africa unless we act now. This would represent a return to mortality levels last seen 20 years ago - and children and pregnant are likely to be hardest hit.
But if we work together to ensure malaria prevention, detection and treatment measures continue during the COVID-19 outbreak; we can reduce the pressure on weak health systems and give them the best chance to respond. This means ensuring countries do not scale back mosquito control activities, such as insecticide-treated nets and indoor residual spraying, that chemoprevention for pregnant women and young children is maintained, and people living in places with malaria who develop a fever seek diagnosis and care as soon as possible.
These investments don’t just tackle malaria; they also help strengthen the resilience of the wider health system, building up capacity and infrastructure that can provide an invaluable foundation for other eradication programmes or disease outbreaks, helping to ensure that all people in malaria-affected countries have access to quality healthcare and countries are better prepared to tackle potential future pandemics.
As countries rightly look to take measures to prevent the spread of COVID-19 we have to do all that we can to make sure that planned malaria prevention - such as bed net distribution - and access to antimalarial treatment don't get disrupted, otherwise the knock on consequences will be grave in terms of young lives lost to malaria. The UK and other government’s generosity to The Global Fund to Fight AIDS, TB and Malaria means vital support is available to countries already fighting malaria at scale. Right now the focus must be on making sure that these vital malaria measures go ahead as planned, and front line health workers have all the help they need to manage the multiple threats to the people they care for.